The Relevance of Pupil Size to the Results of a Pupil Evaluation
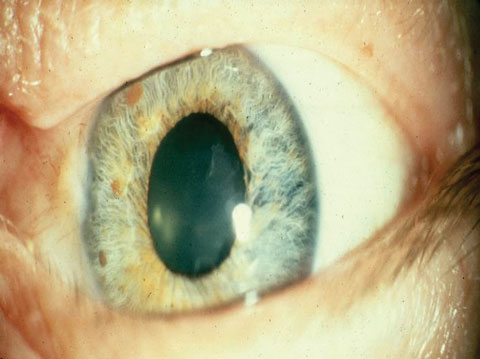
When a doctor examines a patient’s pupils, they might learn a lot about their health. For instance, a person’s pupil diameter measurement may be used as an indicator of whether or not they have had a traumatic brain injury.
Strokes and brain tumors are only two examples of illnesses that may be diagnosed with a thorough pupillary exam.
The question, therefore, becomes, why does pupil size matter when gauging a person’s reaction? This post will look at what each size signifies for the patient’s well-being.
Does having varying pupil diameters indicate something abnormal?
They should both have the same light response in that both pupils widen. Failure to do so may indicate neurological or ocular pathology. Evaluation of the pupils is one method neurologists use to diagnose anisocoria and assess the health of the optic nerve, which transmits visual information from the eyes to the brain.
When is anisocoria normal?
Anisocoria may occur in three distinct forms: the normal, the physiological, and the pathological.
It is considered normal anisocoria when one pupil is bigger than the other, but both pupils still respond correctly to light. It’s typical and typically goes away by itself.
When there is a disparity in pupil size because of a percent change in pupil size, we call this physiological anisocoria. This results in a dilated pupil on one side and a narrowed pupil on the other.
One of the signs of pathologic anisocoria is an abnormal response to light by both pupils, with the bigger pupil being the cause of the problem. This may indicate a more severe problem, such as inflammation or a head injury.
How can the doctor determine whether anisocoria is because of an underlying medical problem?
When a patient presents with anisocoria, a medical professional may get a better idea of the cause by examining the patient’s pupils. A neurologic assessment and a visual acuity test might be part of this checkup.
The doctor will use a pupilometer or a neurological pupil index test to determine the exact diameter of each pupil in both eyes.
Health experts may evaluate the light sensitivity of the eyes with the use of a pupilometer. The doctor will also check out what you can see when you stare straight ahead, known as the “visual field.” It is possible that a retinal issue or brain damage is to blame for the patient’s reduced vision and anisocoria.
How do the experts know if the pupil is “too big” or “too small”?
To properly evaluate anisocoria, you must first determine which pupil has the bigger pupillary distance. Pupils enlarge in dim light; something could be wrong if the miotic pupil isn’t reacting normally. Anything may be wrong if your bigger (mydriatic) pupil doesn’t narrow when exposed to intense light (or growing smaller).
What causes an abnormally large (dilated or mydriatic) pupil?
If the eye injury has injured the iris tissue, the pupil may not react properly to intense light and stay open (i.e., a concussion). There is a possibility that Adie’s tonic pupil syndrome is a contributing factor.
It is more common in young adult women and often begins in one eye. People often complain that their pupils respond too slowly to light. Patients with this illness often struggle to pay attention to nearby objects because their deep tendon reflexes are impaired.
The illness often does not cause serious health problems. Pupil dilation may be achieved using eye drops, nasal sprays, or other drugs. Wipes containing an antiperspirant meant for another use might temporarily dilate the pupil if placed in the eye.
Finally, issues with the third cranial nerve, which transmits signals between the brain and the eye, may lead to abnormal pupils. The third cranial nerve controls blinking and eyelid movement. Ptosis, drooping of the top eyelid, and a widened pupil are common signs of this illness.
A physician might wish to request emergency brain imaging investigations for a patient with third cranial nerve palsy to rule out more severe issues.
What are some causes of an abnormally small (miotic) pupil?
A miotic pupil may arise from several different conditions. Horner’s syndrome is the most typical, and it is brought on by injury to the sympathetic nerve fibers that go from the spine to the eye.





